
19 Mar My child has croup: what can I do?
What do I need to know? asks Thea van de Mortel
With the surge in Omicron cases, doctors are finding presentations of croup in children seeking hospital care for COVID in Australia and internationally.
In some cases, children presenting to hospital with croup are infected only with SARS-CoV-2, the virus that causes COVID.
In other cases, they’re co-infected with SARS-CoV-2 and another virus that typically causes croup.
What is croup and what are the symptoms?
Croup (laryngotracheobronchitis) occurs when there is inflammation and swelling in the upper respiratory tract of young children (usually aged under five years) in response to a viral infection.
The most common cause is the parainfluenza virus. Other culprits include adenoviruses and respiratory syncytial virus (RSV).
A typical sign of croup is a barking cough, which sounds like a seal or barking dog.

Croup is more common in boys and typically lasts about three to five days.
Croup often presents initially as a respiratory tract infection, with a runny nose, sore throat, cough and fever.
As the inflammation progresses, the inflammatory chemicals that are produced cause capillaries (small blood vessels) to leak fluid, leading to swelling of air passages in the larynx (voice box), trachea (windpipe) and the bronchi (upper airways of the lungs).
Because young children have narrower airways than older children and adults, this swelling can lead to partial airway obstruction, particularly in younger or smaller children.
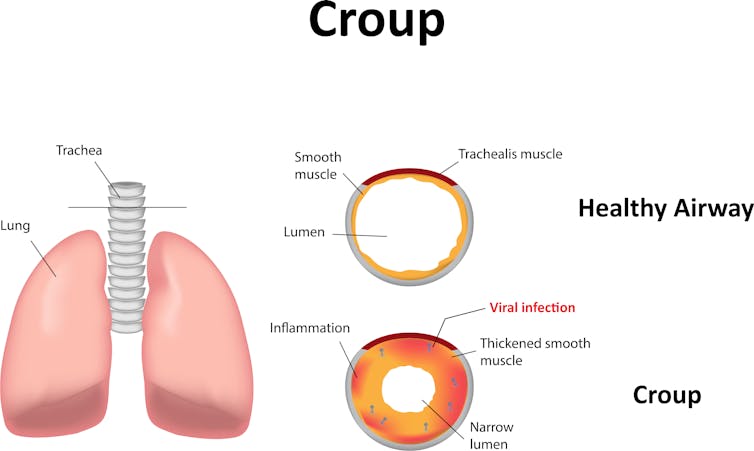
Shutterstock
This may lead to inspiratory stridor (a high pitched noise when breathing in) and increased work of breathing.
Their respiratory rate (number of breaths per minute) may increase and they may show signs of increased respiratory effort, for example, their nostrils flaring when taking a breath, and the area at the base of the throat sucking inwards when breathing in (tracheal tug).
As it gets more difficult to breath, the child uses their tummy muscles and muscles between their ribs to help them breath. They may also become anxious or distressed.
Why might croup be related to COVID?
Anything that causes inflammation and swelling in the upper airways of small children can lead to croup symptoms.
The Omicron variant, like the typical viruses that cause croup, is also a respiratory virus.
And unlike the Delta variant, Omicron causes causes most of its inflammation in the upper airways rather than the lungs.
Croup from illnesses other than COVID is typically more common in autumn and winter.
How is croup treated?
Mild croup – where your child does not have breathing difficulties and is able to eat and drink – can be managed at home.
Fevers and sore throats can be treated with ibuprofen (in children over three months of age) or paracetamol. Your doctor may also prescribe a steroid medication to reduce inflammation.
Make sure your child has plenty of fluids as they will lose fluid through fever.
Keep your child as calm as possible as crying and distress make the condition worse.
If the symptoms become worse, in moderate croup, steroids are used to reduce inflammation and swelling.
In more severe cases, children are given nebulised adrenaline, which works rapidly to reduce airway swelling.
Prevention of croup relies on preventing viral infections, so practice good hand hygiene and respiratory etiquette (coughing into your elbow).
Other measures to prevent SARS-CoV-2 infection include vaccination of eligible family members, good ventilation at home (get a good through draft with doors and windows open where possible), and having kids play outdoors.
When to see a doctor or call an ambulance
Seek immediate medical advice if your child is having trouble eating or drinking, showing signs of respiratory distress, is sick for more than four days, or aged less than six months of age. Or if you’re concerned for another reason.
(For a more complete list of when to see a doctor for croup, see the government’s Healthdirect fact sheet).
Call an ambulance if your child is struggling to breathe, becomes pale and drowsy, looks very sick, starts drooling or can’t swallow, or develops cyanosis (blue lips).![]()
Thea van de Mortel, Professor, Nursing and Deputy Head (Learning & Teaching), School of Nursing and Midwifery, Griffith University
This article is republished from The Conversation under a Creative Commons license. Read the original article.

