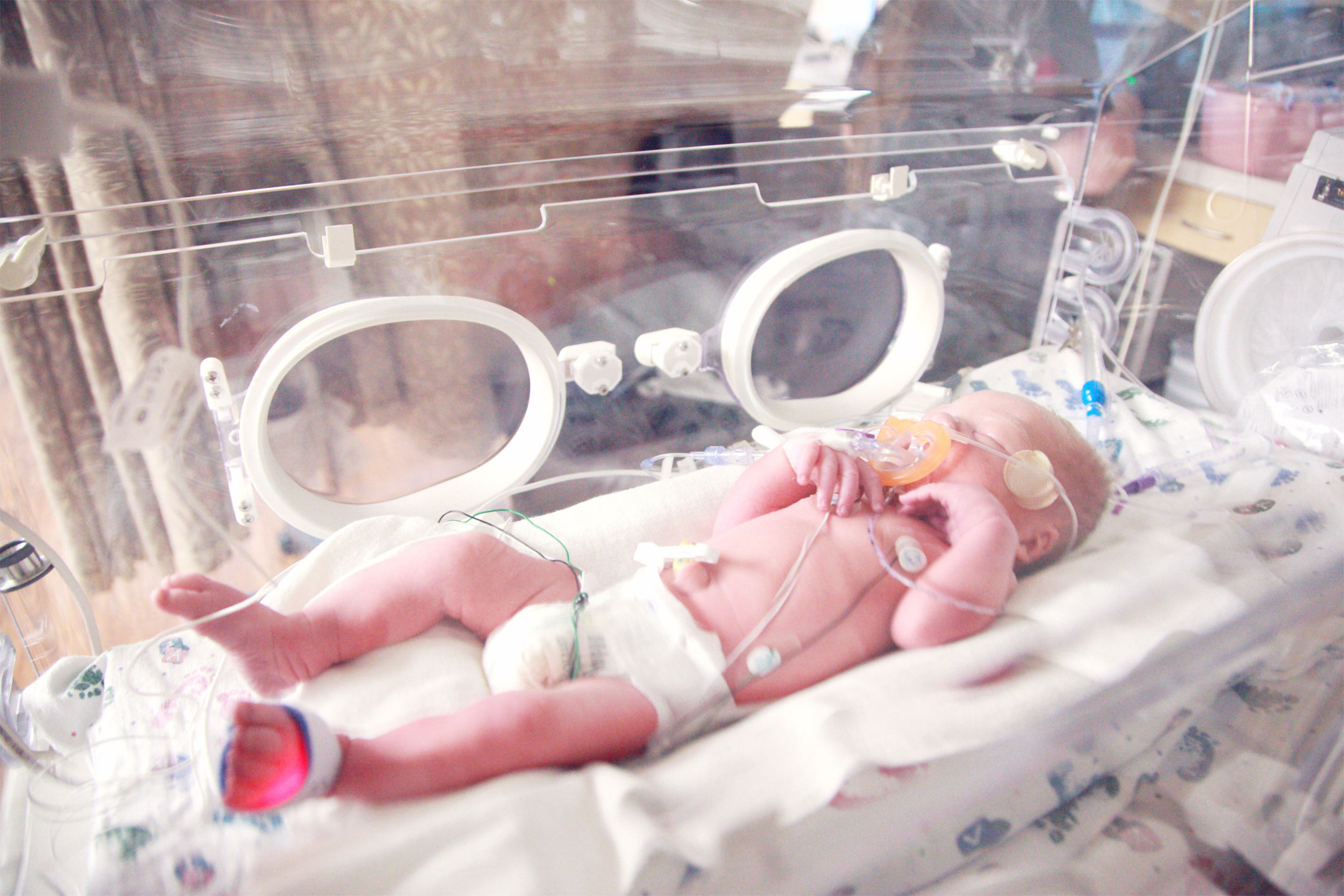
06 Jul New Guidelines introduced to Support Very Preterm Babies
New Guidelines to Support Very Preterm Babies
Australian health experts have introduced groundbreaking guidelines to enhance the long-term health outcomes of children born very preterm. These clinical practice guidelines are the first of their kind in the country, focusing on the care of babies born before 32 weeks’ gestation from hospital discharge until six years of age.
Led by the Murdoch Children’s Research Institute (MCRI)’s Centre of Research Excellence in Newborn Medicine, the guidelines were developed with input from neonatologists, pediatricians, clinicians, maternal and child health nurses, and those with lived experiences of preterm birth from across Australia.
Professor Jeanie Cheong from MCRI emphasized that these guidelines recommend structured post-discharge care for very preterm babies who are at increased risk of growth, health, and developmental problems. Each year, about 3,500 babies, or 1.1 percent of all births in Australia, are very preterm, and around 60 percent of these children will face challenges.
“Children born very preterm need intensive medical care to survive,” said Professor Cheong. “Although treatment has advanced and survival rates have improved, these children still face potential health issues such as delayed growth, elevated blood pressure, hearing loss, neurodevelopmental and sleep problems, language delay, and autism. Some difficulties appear early in life, while others emerge during the preschool years. Very preterm birth is distressing for caregivers and families, adding to the carer burden and impacting family wellbeing, mental health, and quality of life.”
Professor Cheong noted that follow-up services for these children vary significantly across Australia, leading to inconsistencies in care. “A lack of consistency in follow-up care at hospitals and other medical and community services means many children miss out on important assessments and timely referrals. It’s crucial to identify difficulties early to ensure children receive appropriate early intervention.”
Dr. Jamie Owen from MCRI stated that to avoid gaps in care, every family with a very preterm child should be supported by a coordinated, multidisciplinary team. “These guidelines detail how GP clinics, hospitals, and healthcare centers can collaborate to ensure all children have access to ongoing care, with any health concerns identified and treated early. Follow-up care should be tailored to each child and initiated by the hospital’s Neonatal Intensive Care Unit (NICU) team. This often involves multiple healthcare professionals and services, making coordination essential to maximize efficiency, reduce duplication, and lessen the burden on families.”
One compelling story highlighting the importance of these guidelines is that of Teddy, born at just 26 weeks’ gestation, weighing only 719 grams—about as much as a glass of milk. Teddy’s mother, Sarah Kirby, recalled the emergency caesarean performed when Teddy’s heart rate slowed. Teddy spent nearly 100 days in the NICU, needing breathing support and a feeding tube. “Everything happened so quickly, and it was hard to process that he wasn’t going to be born full term,” Sarah said. “When I first held him, he was about the size of my hand.”
Despite the challenging statistics for very preterm babies, Sarah expressed immense gratitude for Teddy’s progress. Now 14 months old, Teddy is cheeky, inquisitive, and only requires physiotherapy. “Many preterm babies take one step forward and four steps back, but Teddy hasn’t had many setbacks. He has reached all the required milestones and is the light of our lives.”
Sarah finds the new national guidelines incredibly reassuring. “Being a mum of a preterm baby is overwhelming, so having structure and access to the right supports once you leave the hospital is invaluable. This will be a huge comfort to families, knowing their babies will have the best follow-up care.”
These guidelines, approved by the National Health and Medical Research Council (NHMRC), will be reviewed and updated with additional evidence-based recommendations every five years. Professor Cheong highlighted that further funding could help extend follow-up care for preterm children throughout their schooling years and into adulthood.
For parents of very preterm babies, these new guidelines offer hope and assurance that their children will receive the comprehensive care needed to thrive.

